Headaches: They live on a spectrum from “mild inconvenience” to “serious health condition,” and it seems like there are a thousand possible causes.
While it’s difficult to pin down the exact cause of every headache, research shows that 60% of people who experience migraines at least perceive themselves to be sensitive to weather conditions while keeping a headache journal.
People who experience weather-related migraine headaches are like human barometres — they can feel changes in atmospheric pressure before they manifest. But how do you really know if it’s the weather causing your headache?
Barometric pressure headaches: How air pressure causes them
Migraine weather: You’ve probably heard the term, but what does it actually mean? How do weather changes affect headaches?
The air around you carries a certain weight, and it’s called atmospheric pressure. Atmospheric pressure, measured by a barometer, fluctuates with the weather. When a low pressure weather system moves into your area, wind and rain follow.
Your sinuses are filled with air. When there’s an imbalance between the pressure in your sinus cavities and the air pressure outside, you can feel some pain due to the fluctuations in atmospheric pressure. Your blood vessels may constrict, and the neurons in your trigeminal nucleus may be firing — all causing discomfort.
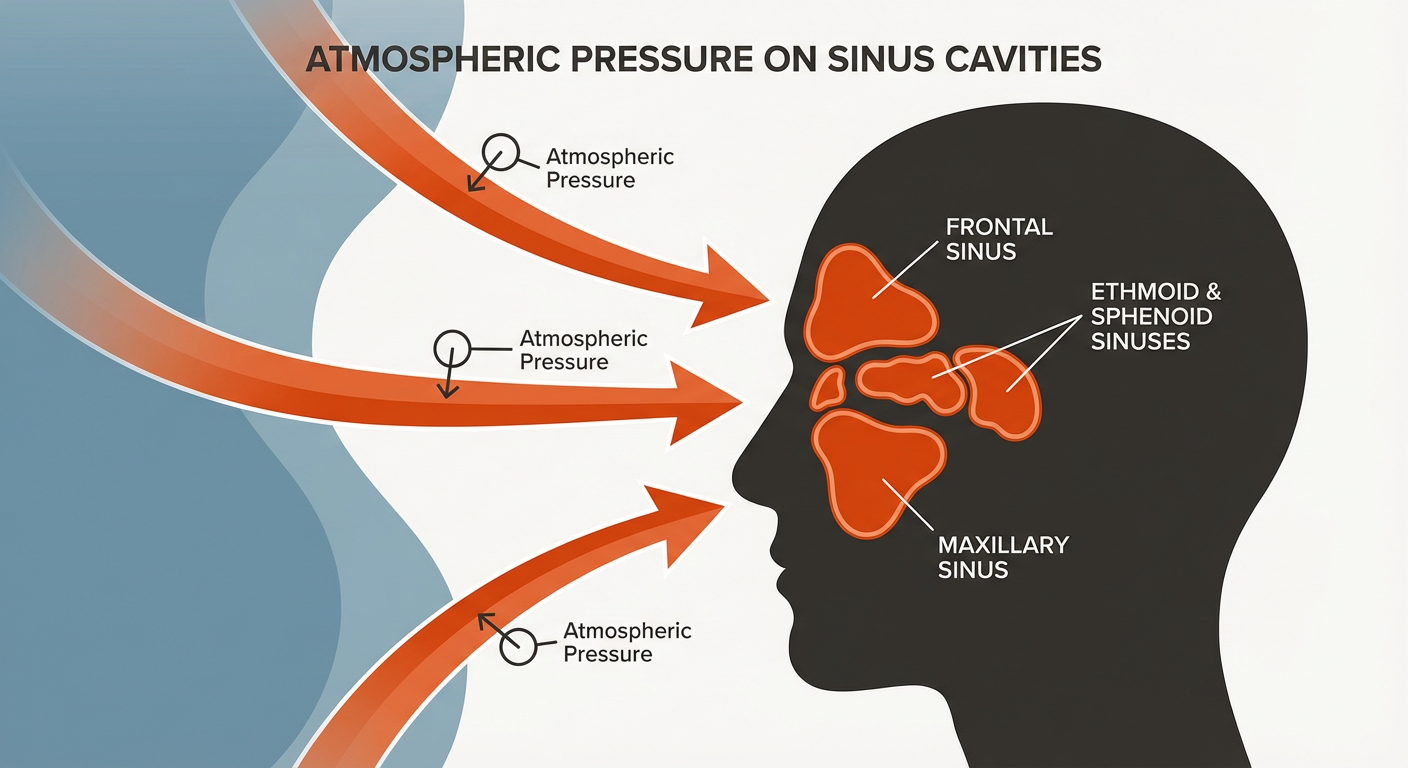
You can experience a headache due to changes in barometric pressure when:
- Outside temperature or humidity suddenly changes
- There’s a storm outside
- You take off in a plane
Is it a weather pressure headache? Signs and symptoms
First: You should see a doctor if you’re concerned about your headaches, regardless of the cause.
But without some data collection, a doctor won’t be able to tell you definitively that your headaches are caused by the weather. This is because some people who experience barometric pressure headaches notice their symptoms before the weather changes, and the correlation may be difficult to pin down.
A barometric pressure headache can look like a migraine headache, which is associated with the following symptoms:
- A headache that lasts between four hours and three days
- Sensitivity to light
- Visual disturbances, such as auras
- Nausea and vomiting
- Diarrhea
- Depression or anxiety
- Dizziness
- Excessive yawning
- Changes to speech
- Memory and concentration issues
- Insomnia
- Food cravings, which can worsen symptoms
Quick tip: Keep a headache journal
The best way to determine if your headaches are caused by pressure changes is to keep a headache journal. Every time you have a headache, note the date, time, symptoms, length of the headache, and the pressure changes in weather.

If you begin to notice a pattern that points to weather as a trigger for your headaches, bring your journal to your doctor to discuss the correlation.
Your doctor may ask more questions and consider ordering tests based on your history before feeling confident that you’re experiencing barometric pressure headaches.
Treatment options for weather change headaches
If your headaches are manageable, over-the-counter pain medication such as ibuprofen or acetaminophen may be your best bet. You may want to try a mix of aspirin, acetaminophen, and caffeine — but speak with your doctor first before taking any medication on a regular basis.
But if your headaches are affecting your quality of life, your doctor will be able to prescribe migraine medication, usually triptans, to help with severe symptoms.
Triptans
Triptans block pain pathways in the brain, and they can be taken as pills, shots, or nasal sprays.
Common side effects include:
- Tingling or burning of the skin
- Numbness
- Dizziness and/or drowsiness
- Dry mouth
- Headache
- Nausea
Triptans shouldn’t be taken with ergotamines (see below), nor if you’re at risk of heart disease, stroke, or diabetes.
At-home treatment options for barometric pressure headaches
The best thing you can do at home when you have a headache or migraine is to get a lot of rest.
Avoid alcohol, limit physical activity, stay hydrated, and take a warm bath.
While there are no foods or supplements that can alleviate an acute migraine attack, it does help to know your own triggers.
Keep a lifestyle journal that documents your food intake, stress levels, and possible weather triggers so that you know, over time, how to avoid certain factors that may trigger a headache.
Can you prevent a barometric pressure headache?
Barometric pressure headaches are rough because you can’t avoid atmospheric pressure. We’re all at the mercy of the weather. So what are your options?
First, start with the basics of overall good health:
- Stay hydrated
- Document and avoid food triggers
- Get a solid eight hours of sleep every night
- Try to keep your stress under control with meditation
- Exercise on a regular basis
- Eat a well-balanced diet full of fruits and vegetables
- Avoid alcohol, smoking, and caffeine if this is a trigger
If you feel like you’re living a relatively healthy lifestyle, however, and you need more ammunition against your headaches, there are some additional steps you can take:
Magnesium
A 2017 systematic review of clinical trials published between 1990–2016 found that magnesium is “possibly effective” for the prevention of migraine headaches.
But keep in mind that only five trials out of 204 met the review’s criteria, meaning more research is needed to be sure. You may not even need a supplement if you’re eating nuts, seeds, whole grains, beans, leafy vegetables, and yogurt, which are natural sources of magnesium.
Beta-blockers
Some beta-blockers have been found to reduce episodic migraine headaches by 1.5 headaches per month after eight weeks of treatment.
Side effects may include:
- Fatigue
- Dizziness
- Cold fingers or toes
- Insomnia
- Nausea
Botox
Botox isn’t just for cosmetic use — Botox has been authorized for sale by Health Canada for chronic migraines in 2011.
Nerves communicate pain by releasing molecules to sensory organs. Botox prevents this communication from happening, which can be extremely helpful for people who suffer from chronic migraines.
Keep in mind that your migraines need to be severe for your doctor to prescribe Botox, and they will likely try magnesium or beta-blockers before trying Botox. Chronic migraine sufferers have more than 15 days of headaches per month for at least three months.
When to see a doctor for your headaches
Most of the time, you don’t need to worry if you have a headache. But if you experience any of the following symptoms, get yourself to a doctor immediately:
- A severe headache with sudden onset
- Severe symptoms that don’t respond to medication
- Fever
- Blood in your stool
- Muscle weakness or numbness
- Vision or speech changes that persist after the headache
- Memory loss or confusion
- Neck stiffness
- Any neurological symptom
These symptoms are signs that your headache is not caused by the weather — it could be a stroke or aneurysm. And atmospheric pressure is nothing compared to those conditions!
Talk to a doctor who can help
Remember, your headaches may or may not be caused by the weather — but you should seek treatment regardless if they’re affecting your quality of life. Start an online visit with Felix to find out what’s right for you.

