Non-hormonal contraception is any form of birth control that doesn’t affect the hormones of the person using it. There are plenty of hormone-free birth control options that vary by things like cost, effectiveness rate, and duration of protection.
Everyone is different, so there is no one birth control method that will work best for everyone. In this article, we’ll go over all of the different non-hormonal birth control options, along with information on how to access them.
Why choose non-hormonal birth control over hormonal birth control?
There are a number of reasons why you might want to consider alternatives to hormonal methods like birth control pills when looking for a way to prevent pregnancy. Hormonal methods of birth control can have side effects and risks that might not work for your lifestyle. People taking hormonal birth control may also deal with change in mood, decreased libido, and risk of sexual pain.

Get birth control delivered to your door
Fast online assessment with a Canadian nurse practitioner. Choose your method, get your prescription, never run out.
Some non-hormonal birth control options are also more accessible, since they don’t require a prescription. Hormone-free birth control provides choices for people who want to protect themselves against unwanted pregnancy without affecting their hormones.
What are the different kinds of non-hormonal birth control?
In this section, we’ll break down the three main types of non-hormonal birth control: barrier methods, long term and permanent birth control, and behavioural methods.
Barrier methods
Barrier methods are forms of hormone-free birth control that prevent pregnancy by blocking sperm from entering the uterus, creating a physical barrier between the sperm and the egg to prevent fertilization.
External condom
Often referred to as a male condom, an external condom is a protective sheath which is worn over the penis. External condoms are usually made of latex, but they also come in polyurethane or sheep intestine to protect those with latex allergies. Latex and polyurethane condoms protect against sexually transmitted infections (STIs), but sheep intestine condoms do not.
External condoms are widely available without a prescription.
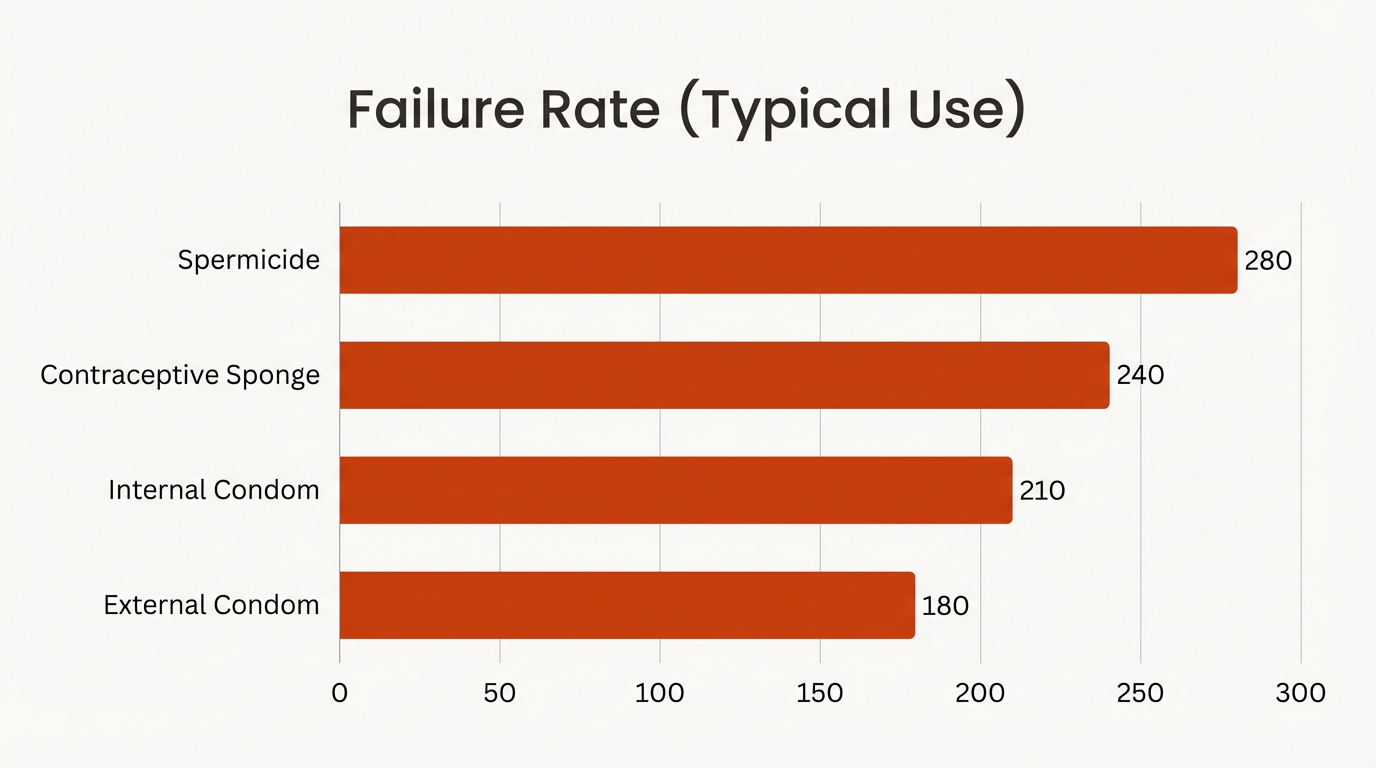
*Failure rate with typical use: 180/1000.
Failure rate with perfect use: 20/1000.
Internal condom
Also known as female condoms, internal condoms are placed inside the vagina prior to intercourse. They are usually made with polyurethane, and provide some protection against STIs. Internal condoms have a ring on either end of the condom, with the closed end being inserted into the vagina to cover the cervix.
You do not need a prescription to purchase internal condoms.
Failure rate with typical use: 210/1000.
Failure rate with perfect use: 50/1000.
Cervical cap
Similar to a diaphragm, a cervical cap is a smaller piece of silicone placed over the cervix before intercourse and used with spermicide. It must be left inside the vagina for at least six hours after intercourse. If you have sex multiple times with the cervical cap, you’ll need to add more spermicide and adjust the position of the cap each time. The cervical cap cannot be used during your period and can irritate the cervix, resulting in urinary tract infections (UTIs).
A cervical cap can be purchased over the counter and does not require a prescription.
Failure rate: There is not yet any data on the effectiveness of the cervical cap and gel that is available in Canada, but some early studies indicate a higher failure rate than other forms of contraception.
Outdated barrier methods
Due to their high failure rates, these previously accepted barrier methods are now considered obsolete. If left in for too long, both the diaphragm and the contraceptive sponge can cause toxic shock syndrome and require medical attention. There is also a risk of allergic reaction to spermicide.
Diaphragm
A diaphragm is a small flexible silicone cup that is placed inside the vagina over the cervix, and used with spermicide. It should be inserted no more than six hours prior to intercourse, and must be left in place for six to eight hours after in order to be effective. A diaphragm will last for one to two years and cannot be used during your period.
You will require a prescription for a diaphragm, and it will need to be fitted to your body by your doctor.
Failure rate: There is insufficient data regarding the effectiveness of the diaphragm with gel that is available in Canada, but previous studies have indicated a higher failure rate than other forms of contraception.
Contraceptive sponge
A contraceptive sponge is a single-use plastic foam sponge that comes already filled with spermicide. It is placed inside the vagina before intercourse, where it covers the cervix and releases spermicide to prevent sperm from entering. It can be inserted up to 24 hours before intercourse and must be left in place for six hours after. The contraceptive sponge is less effective at preventing pregnancy in individuals who have previously given birth.
You do not need a prescription to purchase a contraceptive sponge.
Failure rate with typical use for people who have not given birth: 120/1000.
Failure rate with typical use for people who have given birth: 240/1000.
Failure rate with perfect use for people who have not given birth: 90/1000.
Failure rate with perfect use for people who have given birth: 200/1000.
Spermicide
Spermicide is a chemical that comes in the form of a gel, foam, or suppository and is inserted into the vagina before intercourse. It may come with an applicator, or you can use your finger to apply the spermicide. Some spermicides must be applied 15 minutes prior to intercourse, and you must not douche for eight hours after.
Spermicide can be bought over the counter without a prescription.
The failure rate for vaginal spermicides varies from 18% with perfect use to 28% with typical use, making it one of the least effective forms of contraception when used without an additional barrier method.
Long term and permanent birth control methods
These methods of birth control are most appropriate for people who want long term or permanent protection against pregnancy.
Copper IUD
A copper IUD is a thin copper wire that releases ions, generating an inhospitable environment for sperm to survive. This birth control method can last up to 10 years, making it a good option for those who don’t want to have to remember to use contraception every time they have intercourse. Keep in mind that it will not protect against STIs, and copper IUDs can often make your periods heavier, longer, and more painful.
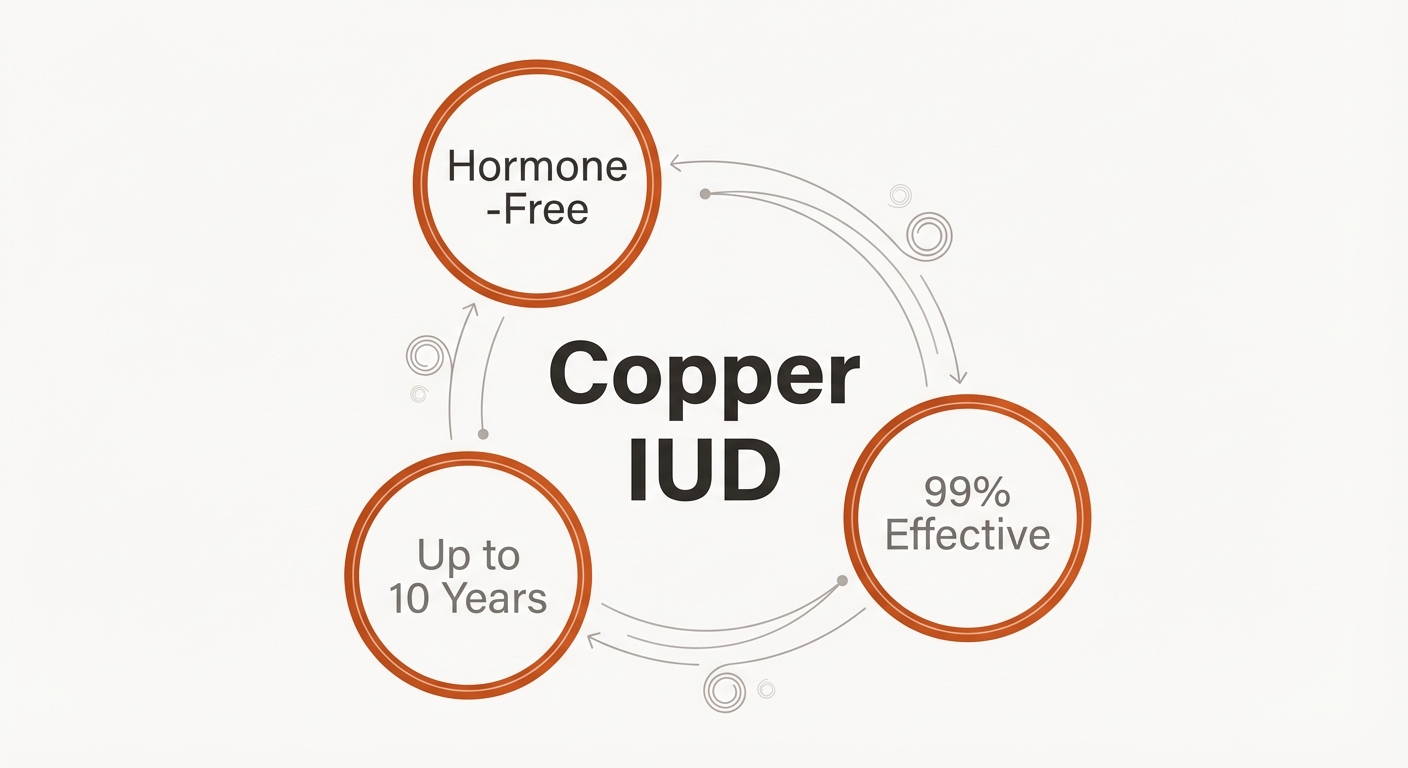
You will need a doctor to insert your copper IUD.
Failure rate with typical use: 8/1000.
Failure rate with perfect use: 8/1000.
Sterilization
Sterilization is a procedure performed by a doctor and is only suitable for individuals who do not want to have children.
Tubal ligation
Tubal ligation, also known as female sterilization, involves the fallopian tubes being cut, removed, or sealed off. It is immediately effective at preventing pregnancy.
Another option is tubal implants or occulsion, which do not require surgery but still provide a permanent solution. Small metal springs are placed in each fallopian tube, causing scar tissue to grow and permanently block the tubes. Tubal implants take three months to be effective at preventing pregnancy. Tubal ligation and implants can be expensive, but they are a one-time cost and are often covered by provincial health plans.
The failure rate for tubal ligation and occlusion depends on the technique used. Talk to your doctor for more information.
Vasectomy
A vasectomy, or male sterilization, is a surgical procedure in which a doctor cuts or seals off the vas deferens tubes, which transport sperm. It takes from two to four months for a vasectomy to become effective at preventing pregnancy. Vasectomies can sometimes be reversed, but there is no guarantee of success, so don’t get a vasectomy unless you are certain you don’t want to have children.
There is also a no-scalpel option for a vasectomy, which uses a clamp to keep the vas deferens closed. It is just as effective as a standard vasectomy, and may cause less bleeding, a smaller hole in the skin, and fewer complications.
Failure rate: 2/100.
Behavioural birth control methods
These methods of birth control require no contraceptives and instead are based on the behaviour of the individuals having intercourse.

Abstinence and outercourse
Refraining from intercourse is the most effective method of preventing pregnancy, but that doesn’t mean you have to give up sexual activity altogether. Non-penetrative sex or non-vaginal sex provide protection against pregnancy and also can reduce the risk of STIs when contact with bodily fluids is limited.
Failure rate: fewer than 1/100.
Withdrawal
Also called the pull-out method, the penis must be removed from the vagina prior to ejaculation. It is a controversial method because it doesn’t prevent pre-ejaculatory fluid from entering the vagina, which may contain sperm. It is also difficult to get the timing right, so emergency contraceptives should be used if withdrawal does not occur before ejaculation.
Failure rate: 4/100 unplanned pregnancies when used exactly as directed.
Fertility awareness methods/natural family planning
Fertility awareness is a form of natural birth control which uses fertility markers to track ovulation daily. By recording indicators like cervical position, cervical fluid, and basal body temperature, you can determine when you are at risk of pregnancy, and only use contraceptives or refrain from intercourse during that time.
Failure rate: 5/100 unplanned pregnancies when used exactly as directed.
Lactational amenorrhea method (breastfeeding)
Breastfeeding as birth control can be an effective method for the first six months after giving birth, provided that your baby is exclusively breastfed. You must be breastfeeding (not pumping) every four hours during the day and every six hours during the night. Once you start ovulating again, this method is no longer effective.
Failure rate: 2/100 unplanned pregnancies or 98% effectiveness when used exactly as directed.
Which non-hormonal birth control options also prevent STIs?
The only birth control methods that prevent STIs are condoms. If you use any contraceptive other than condoms to prevent pregnancy, you should always use an STI protection method as well.
Keep in mind that there are other factors that can impact the effectiveness of your birth control, like antibiotics.
If you’re interested in learning more about hormonal birth control options, check out these articles:
- Which birth control is best for me?
- How long it takes for birth control to work
- When to start birth control pills
- Starting birth control pills on your period
No matter what kind of birth control method you use, there is always a chance of failure. Make sure to follow the directions every single time to decrease the risk of pregnancy, use emergency contraception when necessary, and use additional protection to prevent STIs.
*All failure rate statistics from sexandu.ca.